How to Treat Immune Thrombocytopenic Purpura?
- September 26, 2023
- No Comments
What is Immune Thrombocytopenic Purpura (ITP)?
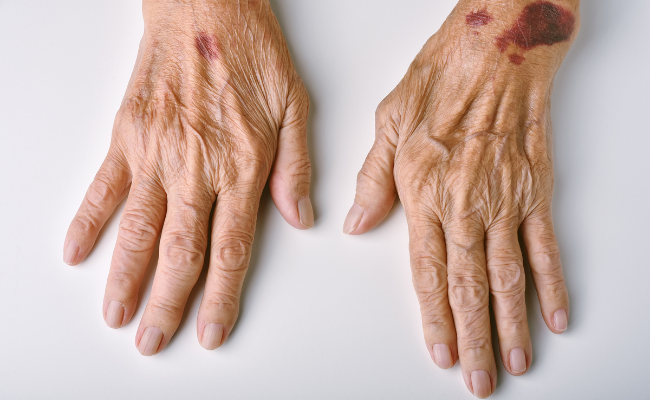
Immune Thrombocytopenic Purpura, commonly known as ITP, is a rare autoimmune disorder that manifests as a significant decrease in platelet levels in the blood. Platelets play a vital role in blood clotting, and their insufficiency can lead to easy bruising and prolonged bleeding, even from minor injuries. ITP is the result of the immune system's erroneous attack on its own platelets, causing their count to fall below normal levels. This condition is often associated with the development of distinctive purple bruises and the presence of small reddish-purple skin spots, resembling a rash.
Why is ITP a Concern?
ITP is a concern due to the potential for severe bleeding episodes. When platelet counts are critically low, individuals with ITP are at risk of spontaneous bleeding, which can be life-threatening if it occurs in vital organs such as the brain. Understanding how to treat ITP is essential to prevent and manage these bleeding episodes effectively.
How to Treat Immune Thrombocytopenic Purpura (ITP)?
The treatment of ITP primarily aims to increase platelet counts, prevent bleeding, and manage the autoimmune response causing platelet destruction. Here's a comprehensive guide on how to treat ITP:
Corticosteroids:
- Corticosteroids like prednisone are often the first-line treatment for ITP.
- They work by suppressing the immune system's attack on platelets, thereby increasing platelet counts.
Intravenous Immunoglobulin (IVIG):
- IVIG is a treatment option for individuals with severe bleeding or when corticosteroids are ineffective.
- It involves infusing immunoglobulins (antibodies) obtained from healthy donors to temporarily boost platelet levels.
Anti-D Immunoglobulin (WinRho):
- This treatment is specifically used for individuals with Rh-positive blood types.
- It works by reducing the destruction of Rh-positive platelets by the immune system.
Platelet Transfusions:
- In cases of severe bleeding or extremely low platelet counts, platelet transfusions may be necessary to raise platelet levels quickly.
Immune Suppressing Medications:
- Medications like rituximab and azathioprine may be prescribed to suppress the immune system's response and reduce platelet destruction.
Splenectomy:
- In cases of severe or chronic ITP, surgical removal of the spleen (splenectomy) may be considered. The spleen is often the site where platelets are destroyed, and removing it can improve platelet counts.
Treatment Solutions:
Effective management of ITP involves several key treatment solutions:
- Individualized Treatment Plans: Treatment plans are tailored to each individual's specific needs, including the severity of ITP and their response to medications.
- Regular Monitoring: Routine monitoring of platelet counts is essential to assess treatment effectiveness and adjust therapy as needed.
- Supportive Care: Supportive measures include lifestyle modifications to prevent bleeding, such as avoiding high-risk activities and using soft toothbrushes to minimize gum bleeding.
- Multidisciplinary Care: A team of healthcare professionals, including hematologists, may collaborate to provide comprehensive care and support.
- Patient Education: Educating individuals with ITP about their condition, treatment options, and potential side effects is crucial for their active participation in managing the disorder.
Benefit Points:
Effectively treating ITP offers several significant benefits:
- Bleeding Control: Treatment helps prevent and manage bleeding episodes, reducing the risk of severe and life-threatening bleeding.
- Improved Quality of Life: By increasing platelet counts and minimizing bleeding, individuals with ITP can enjoy a better quality of life with reduced physical and emotional distress.
- Preventing Complications: Treatment helps prevent complications associated with prolonged bleeding, such as anemia and organ damage.
- Enhanced Mobility: With adequate platelet levels, individuals with ITP can engage in daily activities and exercise without the fear of excessive bleeding.
- Reduced Hospitalizations: Proper management can lead to fewer hospital admissions for bleeding complications, reducing healthcare costs and improving overall well-being.
Comments (0)